Last updated on May 4, 2026

CIGNA HealthCare Prior Authorization Form - IVIG (Intravenous Immune Globulin) 2010-2026 free pr...
pdfFiller is not affiliated with any government organization
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is CIGNA HealthCare Prior Authorization Form - IVIG (Intravenous Immune Globulin)
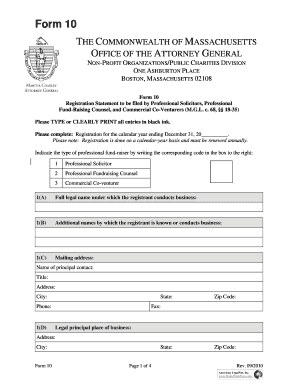
The CIGNA IVIG Prior Authorization Form is a medical consent document used by healthcare providers to obtain prior authorization for Intravenous Immune Globulin (IVIG) treatment.
pdfFiller scores top ratings on review platforms




Who needs CIGNA HealthCare Prior Authorization Form - IVIG (Intravenous Immune Globulin)?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to CIGNA HealthCare Prior Authorization Form - IVIG (Intravenous Immune Globulin)
What is the CIGNA IVIG Prior Authorization Form?
The CIGNA IVIG Prior Authorization Form is essential for healthcare providers seeking authorization for Intravenous Immune Globulin (IVIG) treatments. This form is utilized predominantly for patients diagnosed with specific medical conditions that necessitate IVIG therapy, such as autoimmune diseases, immunodeficiencies, and inflammatory conditions. By requiring prior authorization, insurance companies like CIGNA ensure that the proposed treatments are medically necessary before incurring costs.
Purpose and Benefits of the CIGNA IVIG Prior Authorization Form
This authorization form offers several benefits for both patients and healthcare providers. First, it establishes a clear pathway to secure approval for critical treatments. Patients benefit from streamlined processes that can lead to quicker access to necessary therapies, while providers gain a systematic approach to submitting documentation. Additionally, completing and submitting this form can have significant financial implications, potentially preventing unexpected out-of-pocket costs for patients.
Key Features of the CIGNA IVIG Prior Authorization Form
Key components of the CIGNA IVIG Prior Authorization Form include detailed fields for essential information. Required entries typically feature:
-
Provider and patient personal information
-
Specific medication details including dosage and frequency
-
Clinical justification and detailed patient records
Ensuring that every detail is clear and concise can substantially speed up the processing time for approvals.
Who Needs the CIGNA IVIG Prior Authorization Form?
Various healthcare providers must utilize this authorization form as part of patient care for those requiring IVIG treatments. Typically, patients with conditions such as primary immunodeficiency or autoimmune disorders will need to have this form completed to receive treatment. Prior authorization is particularly crucial in case scenarios where coverage might depend on specific medical necessity criteria established by CIGNA.
How to Fill Out the CIGNA IVIG Prior Authorization Form Online
Filling out the CIGNA IVIG Prior Authorization Form online requires careful attention to detail. Follow these steps to ensure accuracy:
-
Access the form through the designated portal.
-
Complete all required fields related to patient and provider information.
-
Provide detailed clinical justification for IVIG therapy.
-
Review the form for completeness before submission.
Avoid common mistakes, such as leaving fields blank or providing incomplete medical histories, as these can delay processing times.
Required Documents and Supporting Materials
Accompanying the completed CIGNA IVIG Prior Authorization Form, certain essential documents must be included:
-
Clinical records that support the IVIG treatment necessity
-
Medication histories detailing previous therapies
-
Any relevant test results or evaluations
Securing these documents from healthcare providers beforehand can streamline the authorization request process.
Submission Methods and Delivery of the CIGNA IVIG Prior Authorization Form
The completed form can be submitted to CIGNA through several methods. Options include:
-
Online submission via the CIGNA portal
-
Mailing the form to the designated address
-
Faxing the document if preferred
After submission, tracking the status can provide updates on approval, while confirmations will inform you of the next steps in the process.
Security and Compliance for Handling the CIGNA IVIG Prior Authorization Form
When handling sensitive patient information, several security measures are in place to protect data submitted through the CIGNA IVIG Prior Authorization Form. Adherence to HIPAA and relevant regulations ensures that patient confidentiality is maintained throughout the submission process. Proper data protection procedures are crucial for users filling out the form online to mitigate risks associated with information breaches.
How pdfFiller Can Help with Your CIGNA IVIG Prior Authorization Form
pdfFiller offers an array of features that assist users in accurately filling out the CIGNA IVIG Prior Authorization Form. The platform provides tools for:
-
Editing and annotating the form as needed
-
Utilizing eSignature functionality for quick approvals
-
Ensuring secure handling of healthcare documents
Opting for an online platform like pdfFiller can significantly enhance the user experience, simplify form management, and maintain compliance with security standards.
Example or Sample of Completed CIGNA IVIG Prior Authorization Form
To facilitate the completion process, an example or sample of a filled-out CIGNA IVIG Prior Authorization Form can serve as a practical reference. Key elements to note include:
-
Accurate patient and provider information
-
Clear documentation of medical necessity
-
Proper formatting and signatures where required
This visualization can be especially useful for users unfamiliar with the specific requirements of the form, ensuring compliance and accuracy in submissions.
How to fill out the CIGNA HealthCare Prior Authorization Form - IVIG (Intravenous Immune Globulin)
-
1.To access the CIGNA IVIG Prior Authorization Form on pdfFiller, visit the pdfFiller website and log in to your account.
-
2.Use the search function by entering 'CIGNA IVIG Prior Authorization Form' in the provided field to locate the form.
-
3.Click on the form title to open it in the pdfFiller interface, where you will see various blank fields to fill out.
-
4.Before starting, gather all necessary patient and provider information, including relevant clinical records and medication details.
-
5.Begin filling out the form by entering the provider name, patient name, date of birth, and any other required identifiers in the designated fields.
-
6.Utilize pdfFiller's features such as text boxes, checkboxes, and drop-down menus to accurately complete each section of the form.
-
7.Take care to provide comprehensive information to support the prior authorization request and ensure it meets CIGNA's requirements.
-
8.After filling in all sections, review the form thoroughly to check for completeness and accuracy, ensuring all required fields are filled correctly.
-
9.Once you are satisfied with the form, save your changes by clicking the save icon, and consider downloading a copy for your records.
-
10.Finally, follow the submission instructions provided by CIGNA, using the options available on pdfFiller to submit electronically or print for mailing.

Who is eligible to use the CIGNA IVIG Prior Authorization Form?
Healthcare providers who are treating patients requiring IVIG therapy under CIGNA Healthcare are eligible to use this form for prior authorization requests.
What supporting documents are required with this form?
Typically, clinical records, detailed patient information, and medication details are required to support the prior authorization request when using the CIGNA IVIG Form.
How do I submit the completed form?
You can submit the completed CIGNA IVIG Prior Authorization Form through pdfFiller by using the electronic submission option, or by printing it and sending it via mail as instructed by CIGNA.
What common mistakes should I avoid while filling out the form?
Common mistakes include leaving blank fields, not providing enough supporting documentation, and filling out checkboxes incorrectly. Always double-check for completion.
Are there deadlines for submitting the IVIG Prior Authorization Form?
Yes, it is important to submit the form promptly to avoid delays in treatment. CIGNA may provide specific timeframes, so ensure to check with their guidelines.
What is the processing time for prior authorization after submission?
Processing times can vary, but providers typically receive a decision within a few business days after submitting the CIGNA IVIG Prior Authorization Form.
Can patients fill out the form themselves?
While patients can assist in gathering information, the CIGNA IVIG Prior Authorization Form should be completed and submitted by a qualified healthcare provider.
Related Catalogs
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.